COVID Comparisons

Throughout the COVID-19 Pandemic there's been plenty of scary headlines, statistics and tragic individual stories. One thing I've rarely seen, though, is a comparative base for understanding the statistics that drive the scary headlines.
To help with my own understanding, I've compiled a couple of comparable statistics (with sourcing) so I don't have to memorize them, and am publishing them here in case it is helpful for others too.
Key Statistics - Hospitalizations and Deaths per 100K people
First, a disclaimer: I'm not an epidemiologist - I'm just a guy trying to make sense of a lot of important information to make clear-eyed decisions for my family and team in a very charged and dynamic environment.
With this in mind, I generally think about the Pandemic risk in relative terms. Since there's no way to live a full life without risk, I want to understand pandemic risk compared to other things that I see as essential to life or that society has come to accept as "the way things are" (even if it would be great for them not to be this way).
The two most common COVID-related statistics that allow for relative comparisons are measured in Hospitalizations and Deaths per 100,000 (or 100K) people. Other metrics, like the reproduction rate (R0) are useful in other ways, but to understand relative impact on health and mortality, I think these two numbers are the best.
COVID Hospitalizations per 100K
This data is regularly reported in tables of people hospitalized for COVID-19, but often it gets less focus/prominence than the raw number (which is useless unless you know the size of the population) or the change over the prior reporting period (which is interesting, but not for understanding COVID relative to other things).
The CDC provides great data focused on Per 100K numbers in their charts. The screenshot below is from the date I put this post together, and it is updated regularly.
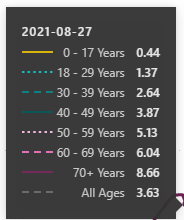

At the time of writing, it was 3.63 for all people in the United States. It ranged from as high was 8.66 for 70+ year olds and as low as 0.44 for <18 year olds.
While this number is changing a lot (and as I write this, Delta is ascendant and there are many media reports of hospitals filling up and oxygen running low), it is important to know this number when trying to evaluate whether COVID is scary compared to other things we've learned to live with.
COVID Deaths per 100K
This data is also regularly reported in tables of people who've died from COVID-19, although international comparisons are often undercounts because they usually only count confirmed cases leading to a fatality. In places where testing is expensive/difficult, then the more accurate academic approach is to look at "excess mortality", but this requires a very long term view and will be mostly useful to academic study into the pandemic over a period of years.
Fortunately, in developed countries where testing is both available and frequent, these numbers are generally a good place to reference on the "per 100K" basis on.
The CDC also maintains a useful dataset for Deaths over time. Unlike the Hospitalizations data (at the time of writing), this chart requires you to choose a Right Axis of Deaths per 100K people over the prior 7 days, since by default it just shows the counts (which while representative of the deep loss of a life and family, aren't useful for comparisons of different things we have come to accept as "part of life").
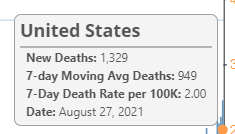

The CDC data allows you to chart up to 6 different regions, but if you want to look at a larger table, a good collation of tabular data is the NY Times COVID Tracker at who at the time of writing have a breakdown under "State trends" with cases over the last 7 days or by all time.
By clicking the row heading for State trends, you can order by Deaths per 100K people over a 7 day period:
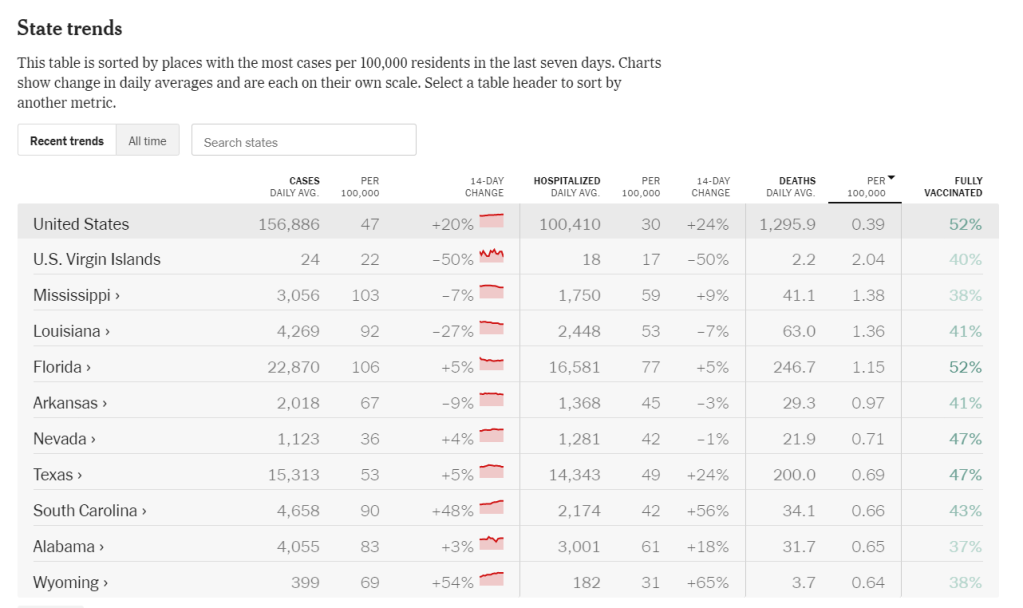
Similarly to Hospitalization data, while this number is changing a lot, and varies significantly by location (because of uneven vaccination rates) and even more by age group, knowing what this number is provides a basis of comparison to other things.
The CDC also provides some lagging data showing the Weekly Deaths per 100K broken down by age group.
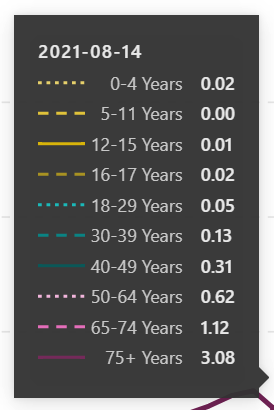
Comparison: Influenza
The most effective comparison - in my opinion - is another regularly mutating virus, spread through the air by people, which has also caused pandemics in the past: influenza.
For the last full year before COVID-19, the CDC produces an estimate of the number of hospitalizations and deaths from Influenza in a detailed report for the 2018-19 United States Influenza season.
Under Table 2 you'll see Hospitalizations and Mortality (deaths) per 100K broken out by age.
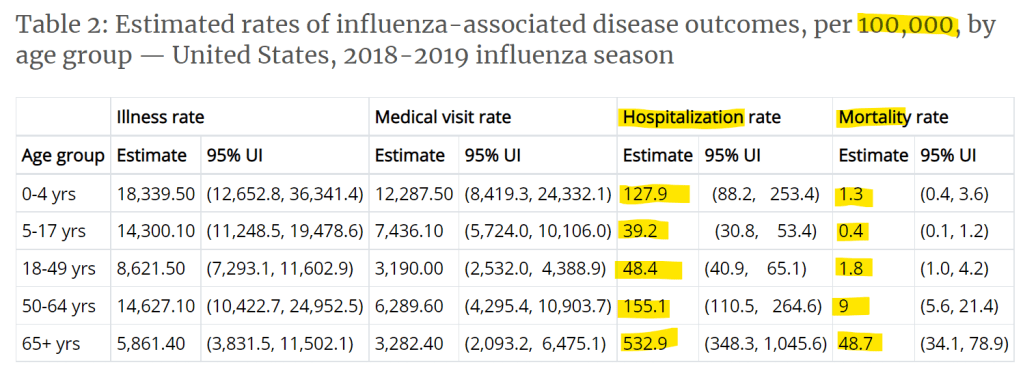
Because this data is only broken out by age group, if we want to have a general comparison, we need to use Table 1 for the "All ages" datapoints. Note in the table below I've removed estimated infections and doctor visits since they aren't part of my comparative set of how scary COVID-19 is.
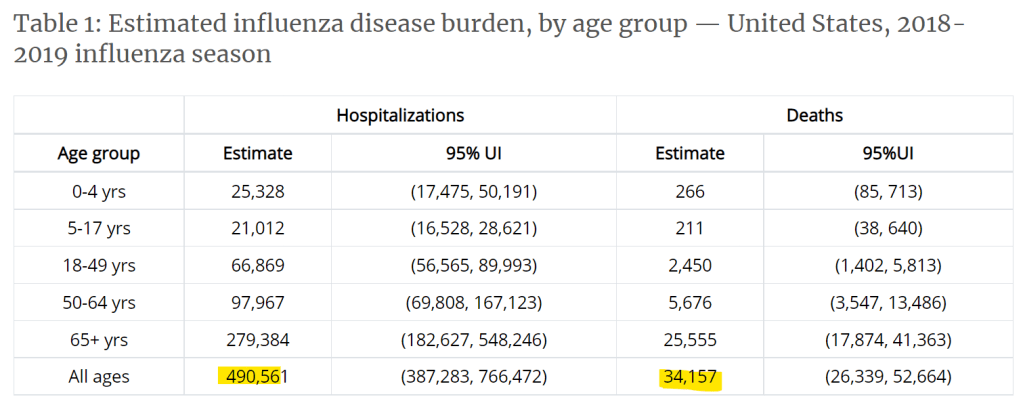
For the 12 month period of 2018-19, the US population was 328.2 million (US Census Bureau).
Since the Influenza data is for an entire season (year), and many of the reports of a highly dynamic pandemic use a trailing 7 day average calculation, we need to try and change the yearly number of a weekly number by dividing by 52. This isn't truly accurate (most influenza hospitalizations and deaths in the US happen in the winter), but it helps to convert a yearly number to a weekly number for comparison purposes.
| Total | Per 100K | Weekly Per 100K | |
| Hospitalizations | 490,561 | 149.47 | 2.874 |
| Deaths | 34,157 | 10.41 | 0.200 |
The key comparative insight is that only weekly COVID Hospitalization rates above 3 and COVID Death rates above 0.2 per 100K people are worse that Influenza.
One other interesting comparison is the age-based Per 100K Hospitalization and Death rates. Using Table 2 Data (which is already Per 100K calculated), converting the Yearly total to a Weekly number shows the following:
| Age group | COVID-19 Hospitalization | Influenza Hospitalization | What's Worse? | COVID Deaths | Influenza Deaths | What's Worse? | |
| 0-4 yrs | 0.44* | 2.46 | Flu 5.5x | 0.02* | 0.025 | Equal | |
| 5-17 yrs | 0.44* | 0.75 | Flu 1.7x | 0.01* | 0.008 | Equal | |
| 18-49 yrs | 1.37-3.87* | 0.93 | COVID 1.5x-4.3x | 0.05-0.31* | 0.035 | COVID 0.7x-8.9x | |
| 50-64 yrs | 5.13-6.04* | 2.98 | COVID 1.7x-2x | 0.62 | 0.173 | COVID 3.6x | |
| 65+ yrs | 8.66 | 10.2 | Flu 1.2x | 1.12-3.08* | 0.937 | COVID 1.2x-3.3x |
* Ages Not Broken Out Equally by CDC COVID Data and Influenza Data
Importantly, the COVID-19 data is incredibly dynamic - I'm using mid-August weekly rates but a better approach would be to use a longer time period (since the numbers for young people in particular bounce between 0 and 0.05, which makes for a different result). However, even using these point-in-time dynamic numbers, it is worth noting that COVID-19 is only 1-2x as likely to put you in hospital as Influenza but it is between 1x and 9x as likely to kill you (with the highest relative impact being for middle-aged folks at this point in time).
At the time of writing,
Comparison: Road Accidents
Another effective comparison which comes from the "risks of living life" is Road Accidents. This national data in the United States is maintained by the National Highway Transportation Safety Board (2019 Report). There aren't good reports for "hospitalizations" but instead "injuries" are tracked which is likely to over-count our comparison with COVID-19 since at least some road accidents are not going to require a trip to the hospital.
| Total | Per 100K | Weekly Per 100K | |
| Injuries | 2.74M | 834.86 | 16.055 |
| Deaths | 36,835 | 11.22 | 0.216 |
Source: NHTSB 2019 and Traffic Facility Data
The key comparative insight is that only weekly COVID Hospitalization rates above 16 and COVID Death rates above 0.22 per 100K people are worse than the risk of dricing in a car on any given day.
As of writing, in almost every State and Territory in the US you're more likely to be Hospitalized for COVID than being injured in a road accident (Florida is worst at 76, and only UT, MD, CO, NY, MI, MN, NJ, RI, CT, MN, NH, MA and VT are below 16), with the national average at 30.
Conclusion
Interestingly - and coincidentally - the risks of dying from Influenza or in a Road Accident are almost the same (0.2 for Flu vs 0.216 for the Roads). You're 5.6x as likely to be injured in a road accident than be hospitalized for Influenza, so to get a good grip on how scared to be of COVID is helps to focus on mortality rates.
The national risk of dying of COVID-19 right now is about twice that of dying of influenza or getting killed in a car accident (0.41 vs 0.22 per 100K), but in 19 states you're actually at lower risk today (MI, UT, IW, ND, WI, NJ, MD, RI, SD, PA, CO, NH, OH, NY, NE, VT, MA, MN, CT and MN).
That said, in the worst affected places you're way more likely to die of COVID than from Influenza or in a Road Accident, such as:
- Mississippi: 1.51 per 100K or 7x more likely
- Florida: 1.22 per 100K or 5.6x more likely
- Louisiana: 1.17 per 100K or 5.4x more likely
- Arkansas: 0.98 per 100K or 4.54x more likely
So, if you're living in a place with a death rate above the chances of catching the flu or going for a drive, you should be scared of COVID. However, if you're not, then you probably should chill out a bit unless you're going to avoid humans and roads forever.
Image Credit: "COVID-19 in Washington DC" by dmbosstone is licensed under CC BY-NC-ND 2.0



